The Duke Congenital Cardiac Surgery Fellowship is a 24-month clinical fellowship designed to develop an autonomous pediatric heart surgeon in the full spectrum of congenital operations. Specific areas of focus include preoperative decision making, operative conduct, and postoperative care.
This is an immersive fellowship where clinicians become part of a highly skilled, compassionate team dedicated to delivering the best care to achieve top outcomes for children and adults with congenital heart disease. The program performs approximately 400 major congenital heart surgeries per year. Following completion of the fellowship, competency is expected in the full range of congenital heart defects and confers eligibility for the congenital cardiac surgery board examination.
Program Director
Duration: 2 years
ACGME approval was obtained for a board eligible congenital cardiac surgery fellowship in 2020, with first entry into the San Francisco match program in 2021. The first anticipated fellow will start July 1, 2022. Approval is for one fellow each academic year.
About the Program
Our educational mission is to train leaders in congenital cardiac surgery who are of the highest clinical caliber and who are committed to careers in which they will continue to advance the field of surgery through research, education, and leadership activities.
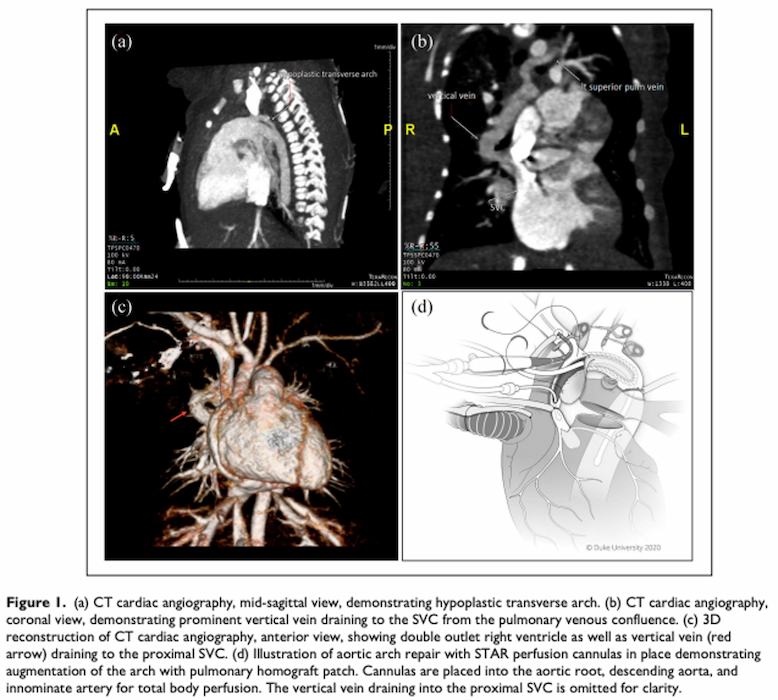
Duke Congenital Cardiac Surgery is a highly innovative program. This includes advancements in all-region perfusion for Norwood operation and arch reconstruction (Sustained total all-region: STAR Perfusion strategy), HAART Aortic Valve Repair Center of Excellence, minimally invasive adult and pediatric congenital heart surgery (PVR, AAOCA, right-sided lesions, VATS epicardial lead placement), and biventricular conversion and biventricular repair. Additional foci of research include thymic co-transplantation for immune tolerance with heart transplantation, and Marfan syndrome aortopathy pathway translational research.

Contact Us
For more information about our program, contact:
Gretchen Lynch, C-TAGME
Program Coordinator
Office: (919) 613-5069
Email: Gretchen.lynch@duke.edu