
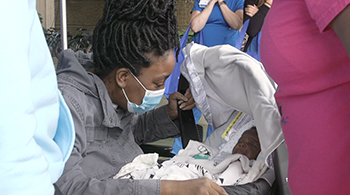
Photo above: Takia Morrison is discharged after recovering from COVID-19
When a baby is born, one of the first people they meet is their mother. For one newborn earlier this year, this was not the case, for his mother, Takia Morrison, was diagnosed with COVID-19. In the wake of the pandemic, caution and the safety of everyone is crucial, and a team at Duke University Hospital was ready to treat Ms. Morrison.
In the Division of Cardiovascular and Thoracic Surgery, Benjamin Bryner, MD, MS, and Jacob Klapper, MD, took charge in the treatment for this case. Even though COVID-19 is new to the world, their experience with various heart and lung therapies have helped in developing a plan to treat COVID-19–positive patients. In this case, the patient had to undergo extracorporeal membrane oxygenation (ECMO), performed by Dr. Bryner, after further complications because of COVID-19.
Proven Therapy
The patient deteriorated quickly, requiring sedation and delivery of her baby by Caesarean section. She was transferred to Duke while her healthy baby remained with family. At Duke, the ECMO device provided respiratory support in tandem with a ventilator. ECMO is a proven therapy for patients with acute respiratory distress syndrome whether it be from the flu, viral pneumonia, or even COVID-19.

Assistant Professor of Surgery, Division of Cardiovascular and Thoracic Surgery
“ECMO is a device that drains blood from the patient’s veins,” says Dr. Bryner. “This drained blood then runs through an artificial lung and finally pumps it back into, in this case, the patient’s vein. This device essentially replaces the work of the lungs.”
At the start of the pandemic there was a lot of uncertainty whether ECMO would be the right treatment for COVID-19–positive patients. To get ahead of the game, Dr. Allan D. Kirk, Department Chair of Surgery, Dr. Joseph Rogers, Chief Medical Officer of Duke University Health System, and Dr. Lisa Pickett, Chief Medical Officer of Duke University Hospital, met with surgeons, the ECMO team, and the medical ICU staff to devise a plan on which treatments would benefit COVID-19–positive patients the most.
“Back in the winter when we knew less about COVID, we spent a lot of time talking with hospital leadership and the intensive care physicians. We’d already considered using ECMO as a viable option, so we started making plans for who we would put on ECMO, and how we would go about doing it safely to protect everybody on the team,” says Dr. Bryner. “This meeting paid off because once the time came, we didn’t have to rush when performing ECMO and the procedure itself went extremely smoothly since we put in hours of preparation beforehand.”
Improved Conditions
Even though ECMO was already considered as a potential treatment early on, the team agreed that using the device would be a last resort. Only a small subset of the population with COVID-19 at Duke University Hospital has undergone ECMO treatment. For this specific case, after the patient’s conditions improved, to further ease her treatment, the team decided to perform a tracheostomy, led by Dr. Klapper.

Assistant Professor of Surgery, Division of Cardiovascular and Thoracic Surgery
“Tracheostomy is moving the breathing tube from the mouth to the throat, which allowed the patient to communicate more and perhaps aided in her coming off of ECMO,” says Dr. Klapper. “Tracheostomy is a nice alternative because it allows for the patient to not only communicate more comfortably, but it will also require less sedation.”
By placing the breathing tube in the windpipe, the patient was disconnected from the ventilator, allowing her lungs to gradually start the work of breathing on their own. This recovery stage was also helped with the use of ECMO and it allowed her to recover faster from COVID-19 in general. With the help of the tracheostomy procedure, the patient was removed from ECMO and her tracheostomy tube was removed after making great progress.
Tremendous Teamwork
Fifty days after Morrison's arrival, a celebratory parade of nurses, physicians and others involved in her care gave her a sendoff as she was discharged. She met her son for the first time just outside the doors of Duke University Hospital, where Morrison's mother rushed to hand over her grandson while Morrison was still in her wheelchair.
The success of the ECMO treatment reflects the tremendous teamwork displayed by the surgeons, medical ICU, nurses, staff, and care teams at regional clinics. For COVID-19–positive patients who require ECMO, time is of the essence, especially if they are transferred from local clinics.
“The key factor that allowed us to have positive outcomes with all of our ECMO patients I’ve had so far is that they were referred to us early enough for the patient to be safely transported here at Duke University Hospital,” says Dr. Bryner. “This was very much a successful collaboration between Duke and other local clinics.”
Give to Duke Surgery
A gift to the Department of Surgery is a gift of knowledge, discovery, and life.