General surgery residents are required to pass the Fundamentals of Laparoscopic Surgery (FLS) and Fundamentals of Endoscopic Surgery simulation-based certifications in accordance with the American Board of Surgery. These simulations develop manual technical skills necessary for successful surgery, but are generally very time consuming, requiring extensive practice to master.
Recently, a team of researchers from the Duke University School of Medicine’s Department of Surgery and Department of Psychiatry and Behavioral Sciences developed and tested a technique that has the potential to accelerate surgeon’s technical skill acquisition. As described in their article published in the journal Brain Stimulation, this study tested if the application of electrical brain stimulation could speed learning as individuals practiced the FLS simulation.
“Currently, residents practice the five FLS tasks in the simulation lab utilizing repetition alone to reach the level of skill required to pass the test,” said Morgan Cox, MD, MHS, lead author and surgical resident. “Given work hour restrictions and balancing clinical duties, we set out to expedite the amount of simulation time required to develop the same level of technical skill.”
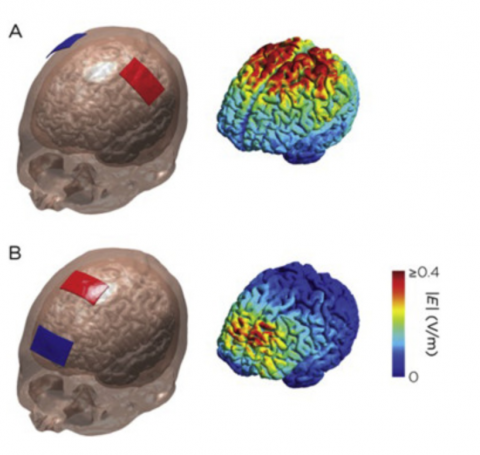
In this study, the authors tested if a form of noninvasive brain stimulation called transcranial direct current stimulation (tDCS) could be applied as individuals practiced laparoscopic surgical skills using the FLS surgical simulator. In this pre-registered, double-blind and placebo-controlled study, sixty participants were randomly divided into three groups: one group who received electrical stimulation over their primary motor cortex, a second group who received electrical stimulation over their supplementary motor area, and a third group who received sham stimulation. These groups each practice the FLS Peg Transfer Task for six 20-minute training blocks with their performance scored based on the number of pegs they transferred, minus penalties for errors.
Results from this study showed that the group practicing with active tDCS delivered to the primary motor cortex produced significantly greater improvement, relative to the group that practiced with sham stimulation. The group that practiced with tDCS to the supplementary motor cortex also showed improvement over the sham group, though this difference did not reach statistical significance.
These results therefore demonstrated that the addition of electrical brain stimulation may improve motor skill learning in a manner that can be applied to speed learning in people looking to gain proficiency in these important surgical simulations.
“It is rewarding that we conducted a well-controlled study that was recognized through publication in a top neuroscience journal,” said Greg Appelbaum, PhD, Associate Professor in Psychiatry and Behavioral Sciences and senior researcher on the study, “however, our next step is to replicate this result and start considering ways that we can implement this technique into surgical training programs”.
In addition to this study from Duke, a research team in Canada led by Drs. Ciechanski, Hecker and Kirton, have found similar results using different, but related designs. Given the successes of both research teams, they are now looking to partner together to replicate and extend their studies, with a particular eye on finding the optimal parameters that produce the greatest gains and longest retention.
In addition to Drs. Cox and Appelbaum, study authors include Zhi-De Deng, PhD, Hannah Palmer, Amanda Watts, Lysianne Beynel, Jonathan Young, Sarah Lisanby, MD, and John Migaly, MD.