
Phone: 919-681-3784
Email: george.kasotakis@duke.edu
Overview
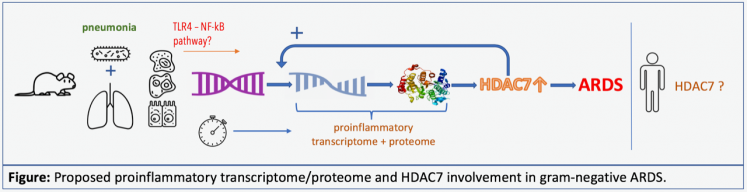
Our research group, under the direction of Dr. George Kasotakis, focuses on the study and application of key concepts in pulmonary inflammation, running the gamut of basic science, translational, and clinical applications. Pulmonary inflammation is a critical process in clearing lung infections and in helping healing after injurious processes; however, uncontrolled levels of it may be harmful to the host, not unlike sepsis. Our group is particularly interested in elucidating the molecular mechanisms and signaling pathways that lead to acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) after stressors are applied to the lungs directly or indirectly.
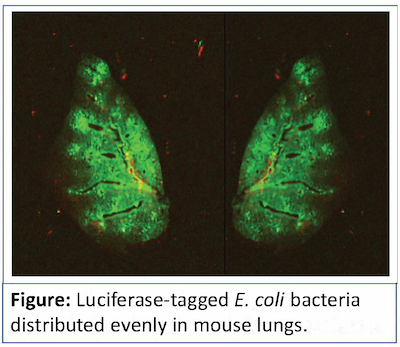
Our group has developed and validated an infectious-based model of murine ARDS with titratable pulmonary inflammation and mortality. With our previous work, we have identified the critical role of a previously unknown enzyme that becomes overexpressed in mice with induced ARDS after gram-negative infection, and the major improvement in inflammation and survival that can be achieved with its timely inhibition. We have also highlighted the dynamic nature of the pulmonary inflammatory immune response and demonstrated the diminishing returns of highly specialized anti-inflammatory therapies over time in ARDS.
Key Projects Underway
- Elucidate the role of TLR signaling in the pulmonary immune response leading to ALI and ARDS.
- Determine the transcriptomic and proteomic changes taking place as ARDS develops, and differentiate a "normal" from an exaggerated immune response after pulmonary infections.
- Understand the intra- and inter-cellular signaling pathways that become activated in pulmonary infections and ARDS.
- Determine the effect of lung inflammation on pulmonary mechanics.
- Determine similarities and differences in the pathways that become activated in the pulmonary immune response between mice and humans.
- Develop sustainable translational strategies to help ameliorate the very high (~40%) mortality seen in patients with ARDS.
- A number of translational and clinical outcomes (non-basic science) projects are also underway in Critical Care, Trauma and Emergency Surgery (please contact for up-to-date list).
Selected Achievements
-
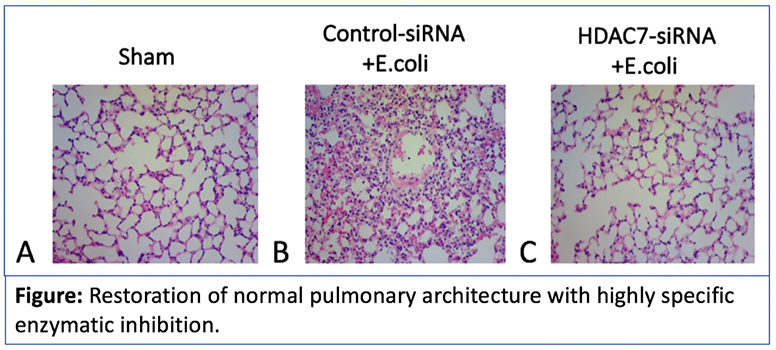
- With our previous work, we have identified the critical role of a previously unknown enzyme that becomes overexpressed in mice with induced ARDS after gram-negative infection, and the major improvement in inflammation and survival that can be achieved with its timely inhibition (PMID 28099388).
- We have highlighted the dynamic nature of the pulmonary inflammatory immune response and demonstrated the diminishing returns of highly specialized anti-inflammatory therapies over time in ARDS (PMID 29180183).
- We have identified the proinflammatory role of activated platelets in the development of ARDS after severe trauma in human patients (PMID 29627883).
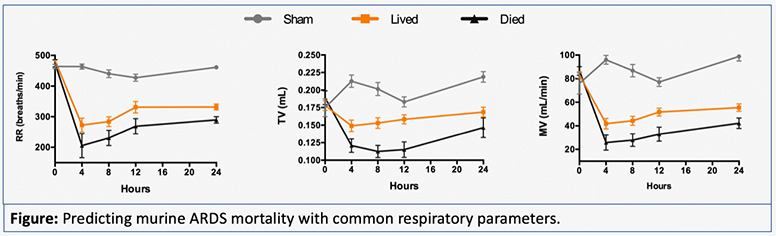
- We have been able to predict mortality in mice by trending common respiratory parameters, such as breath rate and tidal volume.
- This work could not have been made feasible if it was not for our volunteer undergraduate, graduate students and residents who have helped tremendously with several aspects of this work.
- Our work has won several local, regional, and national research distinctions and awards for our volunteer members.
Advanced Training
Research opportunities available for undergraduate and medical students, PhD candidates, residents, and fellows. For more information, please e-mail george.kasotakis@duke.edu.
Contact Us
George Kasotakis, MD, MPH
Assistant Professor of Surgery
Division of Trauma and Critical Care Surgery
Email: george.kasotakis@duke.edu
Publications and Funded Projects
View Dr. Kasotakis's profile to see his publications and funded projects.